 The prognosis is worse in patients who continue to smoke cigarettes or have diabetes mellitus. Approximately 25–30% of patients with critical limb ischemia undergo amputation within 1 year. 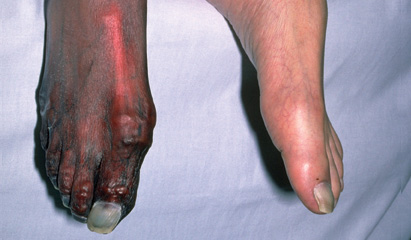
Deterioration is likely to occur in the remainder, with ~1–2% of the group ultimately developing critical limb ischemia each year. Approximately 75–80% of nondiabetic patients who present with mild to moderate claudication remain symptomatically stable. The likelihood of symptomatic progression of PAD is lower than the chance of succumbing to CAD. 
Measurement of ABI is useful for detecting PAD and identifying persons at risk for future atherothrombotic events. Mortality rates are highest in those with the most severe PAD. Patients with PAD have a 15–25% 5-year mortality rate and a two- to sixfold increased risk of death from coronary heart disease. Approximately one-third to one-half of patients with symptomatic PAD have evidence of coronary artery disease (CAD) based on clinical presentation and electrocardiogram, and over one-half have significant CAD by coronary angiography. The natural history of patients with PAD is influenced primarily by the extent of coexisting coronary artery and cerebrovascular disease. ABI values of 0.91–0.99 are considered “borderline,” and those 1.40 indicate noncompressible arteries secondary to vascular calcification. Thus, the ratio of the ankle and brachial artery pressures (termed the ankle:brachial index, or ABI) is 1.00–1.40 in normal individuals. In the presence of hemodynamically significant stenoses, the systolic blood pressure in the leg is decreased. Indeed, ankle pressure may be slightly higher than arm pressure due to pulse-wave amplification. Normally, systolic blood pressure in the legs and arms is similar. Arterial pressure can be recorded noninvasively in the legs by placement of sphygmomanometric cuffs at the ankles and the use of a Doppler device to auscultate or record blood flow from the dorsalis pedis and posterior tibial arteries. An objective assessment of the presence and severity of disease is obtained by noninvasive techniques. The history and physical examination are often sufficient to establish the diagnosis of PAD. Ischemic neuropathy can result in numbness and hyporeflexia. Patients with severe ischemia may develop peripheral edema because they keep their legs in a dependent position much of the time. The time required for rubor to develop or for the veins in the foot to fill when the patient’s legs are transferred from an elevated to a dependent position is related to the severity of the ischemia and the presence of collateral vessels. Elevation of the legs and repeated flexing of the calf muscles produce pallor of the soles of the feet, whereas rubor, secondary to reactive hyperemia, may develop when the legs are dependent. In patients with critical limb ischemia, ulcers or gangrene may occur. .jpg)
With more severe disease, hair loss, thickened nails, smooth and shiny skin, reduced skin temperature, and pallor or cyanosis are common physical signs. Important physical findings of PAD include decreased or absent pulses distal to the obstruction, the presence of bruits over the narrowed artery, and muscle atrophy. With severe ischemia, rest pain may be persistent. Frequently, these symptoms occur at night when the legs are horizontal and improve when the legs are in a dependent position. Patients complain of rest pain or a feeling of cold or numbness in the foot and toes. In patients with severe arterial occlusive disease in whom resting blood flow cannot accommodate basal nutritional needs of the tissues, critical limb ischemia may develop. Symptoms are far more common in the lower than in the upper extremities because of the higher incidence of obstructive lesions in the former region. For example, buttock, hip, thigh, and calf discomfort occurs in patients with aortoiliac disease, whereas calf claudication develops in patients with femoral-popliteal disease. The site of claudication is distal to the location of the occlusive lesion. The most common symptom is intermittent claudication, which is defined as a pain, ache, cramp, numbness, or a sense of fatigue in the muscles it occurs during exercise and is relieved by rest. Fewer than 50% of patients with PAD are symptomatic, although many have a slow or impaired gait. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
